Deft Research recently published the 2020 EMPLOYER/EMPLOYEE GROUP INSURANCE STUDY a survey about workplace health benefits capturing responses from over 800 employers and over 3,000 employees. Among the subjects covered was telehealth. Below are some surprising results.
There are several indicators that would lead us to believe that momentum is increasing for offering more telehealth services to employees. Boosted by the pandemic, employee participation in telehealth has increased from 14% one year ago to 24% as of April, 2020. And rather than offering telehealth as an extra service, employers are more often embedding telehealth in medical benefits – making access and payment for these services easier.
Results from the Employer/Employee Group Insurance Study.
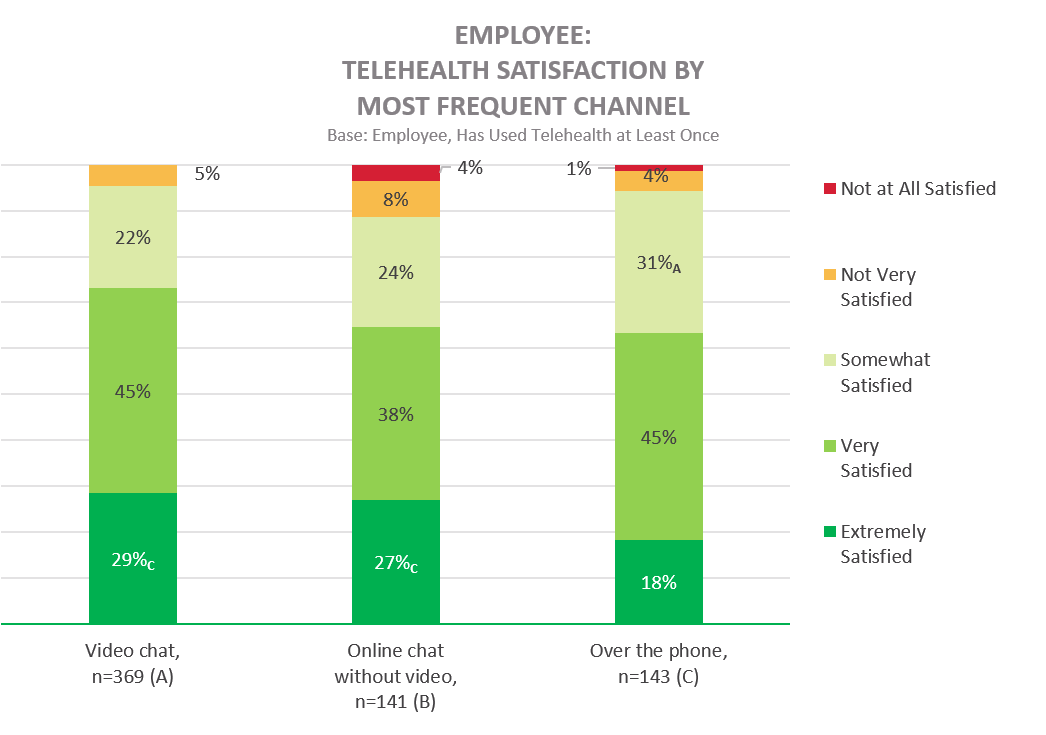
Overall, over 90% of employees who used telehealth services were at least somewhat satisfied with the experience; the majority reported a very or extremely satisfying experience. Satisfaction varied somewhat based on the telehealth delivery channel: the online chat without video channel yields a greater level of dissatisfaction than either video chat or over the phone channels.
BUT, when copayments are added to employees’ considerations, the picture changes. When telehealth copayments are the same as in-person office visits, so there is no financial incentive to use telehealth, only 17% of employees said they would prefer telehealth, 83% preferred an in-person visit.
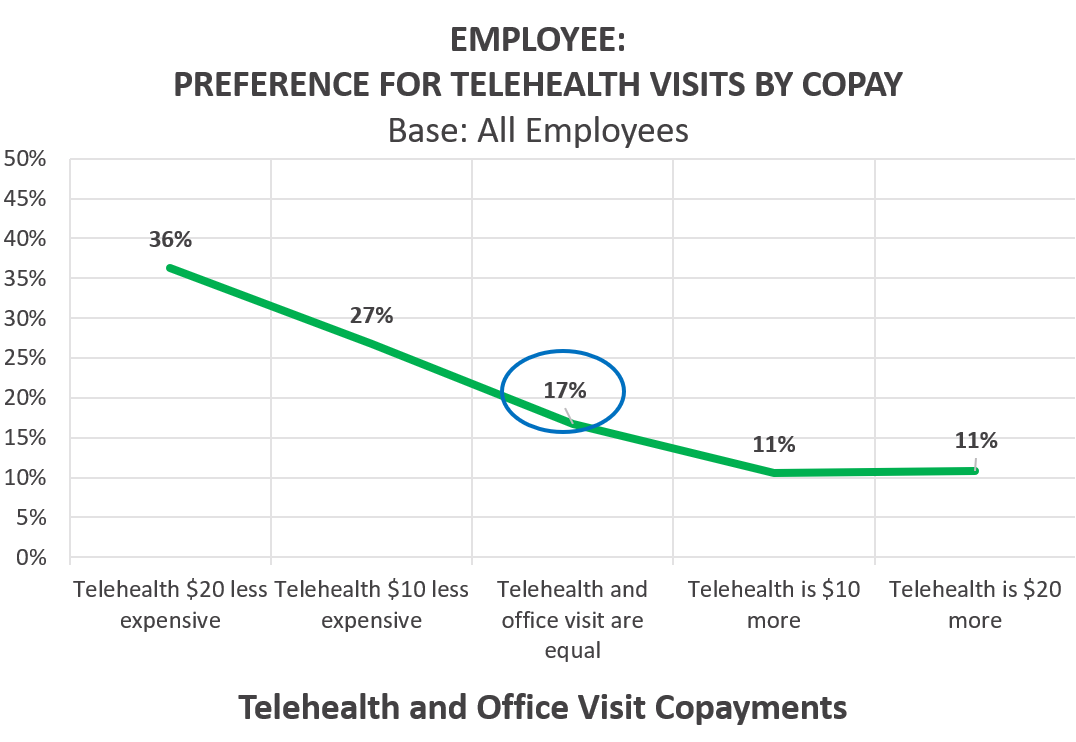
As the chart above shows, when the telehealth copay is $20 cheaper than an in-person visit, preference for telehealth over in-person visits rises from 17% to 36%.
The previous chart showed the preference among ALL employees surveyed, the following chart shows the preference among telehealth users. Among employees that have previously used telehealth, the preference for in-person visits is about the same as it is for the overall employee population. The results illustrate this: when the in-person vs telehealth copay is equal, despite being familiar with telehealth, the majority (81%) of the telehealth users preferred an in-person visit (compared to 83% overall).
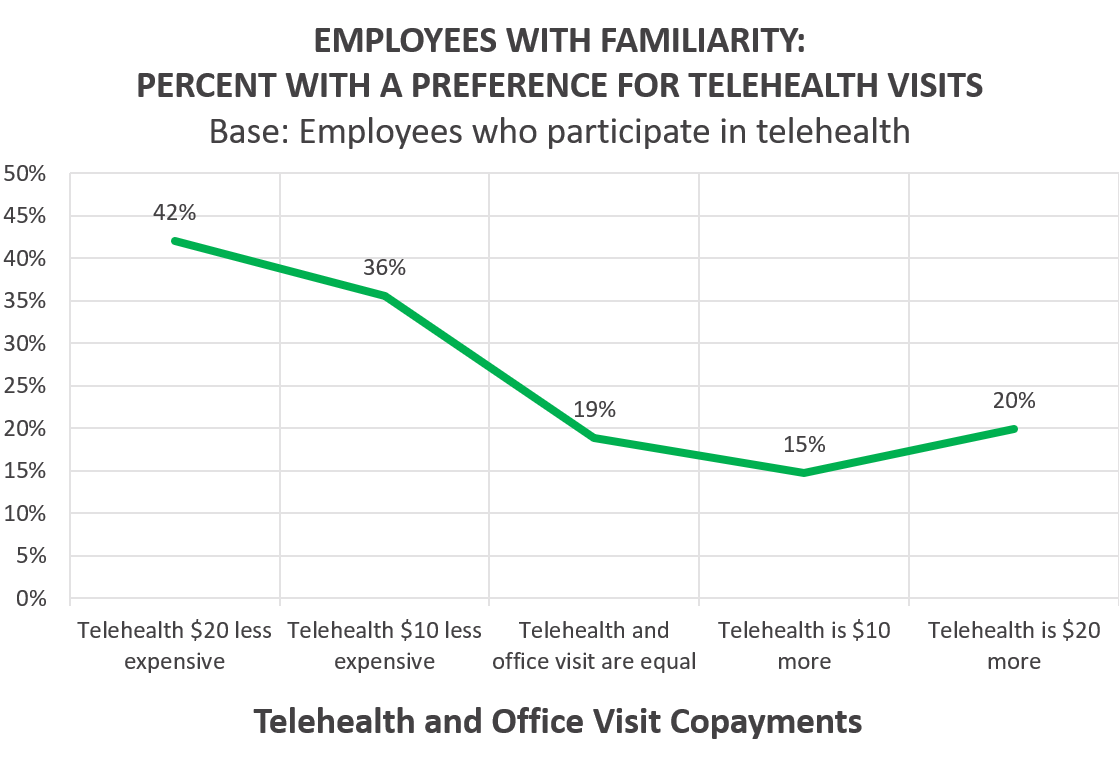
Reaching Patients.
Telehealth might be a good way to engage two types of patients on opposite ends of the health services usage spectrum — those who are not inclined to see a doctor at all, and those who have needed many doctor visits.
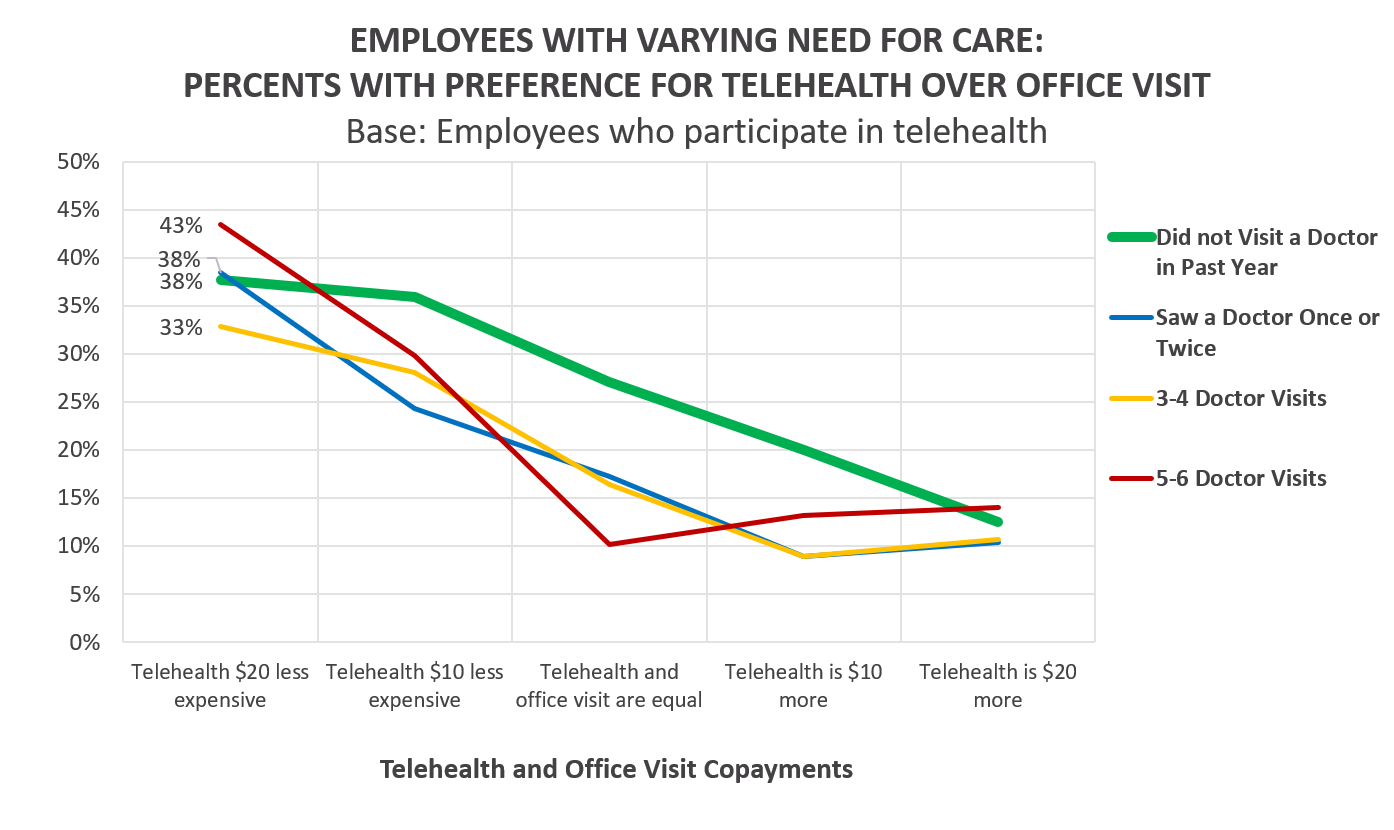
Employees who hadn’t gone to the doctor at all in the past year are more likely to prefer telehealth even when it costs the same as or more than an office visit. According to these findings, a health plan could reach 25% of non-engaged members, or more, by offering them telehealth rather than recommending office visits.
Another group who could benefit from telehealth services are those who have needed many office visits. If they could save $20 on the copay, the study’s results indicate that more than 40% of the least healthy patients would opt for telehealth encounters over in-person visits. In this context, telehealth might serve as a complementary service option for those who require frequent care or monitoring. As a complementary service, cost savings, fewer missed appointments, better monitoring and adherence to treatment regimens, are the promises telehealth potentially fulfills.
Conclusions
When looking at the growth in telehealth volume and the satisfaction it has generated among employees, telehealth benefits clearly have momentum and its time has come. But currently, telehealth alone does not promise a new service improvement that consumers will flock to — there has to be a financial benefit. A key insurance benefit design consideration is the differential in copayment between the in-person visit and the telehealth visit. When copayments are equal, most employees surveyed would prefer a traditional in-office visit. But by offering a copayment differential, the employee preference for telehealth grows substantially.
Familiarity, defined as having experienced telehealth one or more times in the past, does not produce additional preference. The implication is that first-time user incentives to promote telehealth usage may not substantially improve the long-term uptake of the service.
Instead, insurers and employers who want to encourage the use of telehealth services should look at benefit design approaches: 1) financial incentives as discussed above; 2) benefit development aimed at unengaged persons along the lines of incentives and requirements that all have at least a telehealth encounter with a care provider; 3) service development, one focus being to fit telehealth as a complement into the course of care providers deliver to those who need the most care.
Want more insights into Digital Health?
Continuing our coverage of digital health technology, in early August Deft Research will publish a new report titled Usage of Digital Health Tools Study. This study captures the breadth of digital health technology in commercially insured consumers’ lives. The study will cover digital tech’s involvement in delivering general health information, insurance information, use for personal health tracking and monitoring, and use alongside doctors. Sign up for more information here.